In a remarkable medical first, a woman with type 1 diabetes is now living insulin-free after receiving a transplant of islet cells grown from her own fat tissue—reprogrammed into stem cells using only chemicals.
Yes, you read that right: no genes, no embryos—just chemistry and stem cell science converging to rewrite the future of diabetes care.
Reprogramming Cells, Reprogramming Lives
The groundbreaking procedure, carried out in China, used a new generation of chemically induced pluripotent stem cells (CiPSCs). These are adult cells turned back into an embryonic-like state without using viruses or gene editing—just small molecules.
From a small sample of the patient’s adipose tissue, scientists generated CiPSCs, then coaxed them to become insulin-producing islet cells, mimicking the pancreas’s natural function. These lab-grown islets were transplanted under the abdominal wall, not into the liver as traditionally done.
The result? A revolution.

The Patient’s Story: From Crisis to Cure
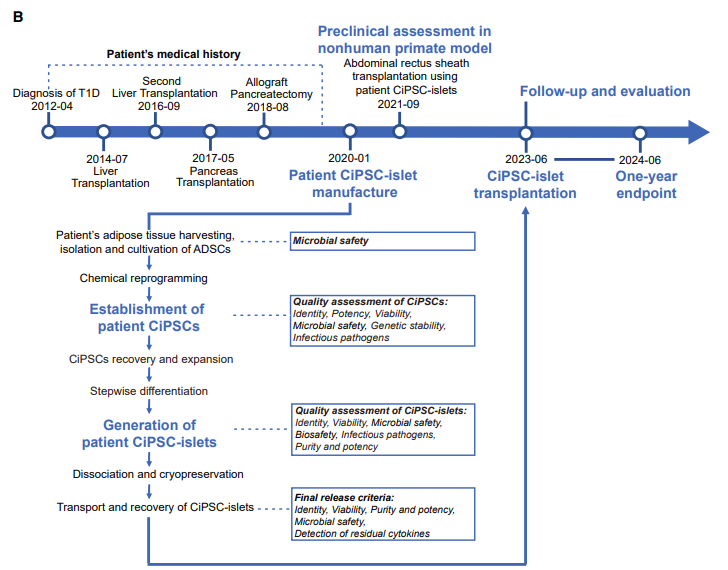
The recipient, a 25-year-old woman with an 11-year history of brittle diabetes, had already undergone two liver transplants and a failed pancreas transplant. Her glucose control was erratic despite heavy insulin use, and she experienced dangerous hypoglycemic episodes.
After receiving the CiPSC-islet transplant in June 2023, her insulin needs began to drop. By day 75, she was completely off insulin. By month 4, 98% of her glucose readings were within the healthy range. Her HbA1c—a long-term marker of blood sugar—fell to a non-diabetic level and stayed there for a year.
What Makes This Different?
This isn’t just a win for one patient—it’s a proof-of-concept for a new kind of personalized medicine.
✔️ Autologous: The cells came from the patient herself—no donor, no rejection risk.
✔️ Chemically induced: Safer and more controllable than gene-based methods.
✔️ Targeted delivery: Transplanting under the abdominal sheath avoided complications linked with liver-based transplants.
✔️ Long-term results: One year later, there’s no tumor formation, no organ damage, and full graft function.
Why It Matters
Type 1 diabetes (T1D) is an autoimmune condition where the body attacks insulin-producing cells. Patients rely on constant insulin injections or pumps—a burdensome, imperfect solution.
The dream has always been islet cell replacement, but that’s been limited by donor shortages, immune rejection, and risk of tumors from stem cell-derived tissue.
This study shows it’s possible to overcome all three hurdles.
Not Ready for Everyone—Yet
It’s important to note that this is a Phase 1 trial with one patient. Safety data beyond one year is still pending, and broader clinical trials are underway.
Moreover, the patient already required immunosuppressants for her liver transplant—so it’s unclear how the therapy would work in someone without prior immune suppression.
Still, researchers say the method is scalable, potentially cost-effective, and well-suited for personalized therapies.
The Bigger Picture: A New Chapter for Regenerative Medicine?
If confirmed in more patients, this therapy could mark the beginning of a paradigm shift—a world where people with autoimmune diseases are treated with cells made from their own bodies, reprogrammed to replace what the immune system has destroyed.
“This is not just a diabetes story,” one scientist noted. “This is a new page in the book of regenerative medicine.”
Reference:
Wang, S., Du, Y., Zhang, B., Meng, G., Liu, Z., Liew, S. Y., … & Shen, Z. (2024). Transplantation of chemically induced pluripotent stem-cell-derived islets under abdominal anterior rectus sheath in a type 1 diabetes patient. Cell, 187(22), 6152-6164.